
He created the ‘Critically Ill Airway’ course and teaches on numerous courses around the world. He coordinates the Alfred ICU’s education and simulation programmes and runs the unit’s education website, INTENSIVE. He is actively involved in in using translational simulation to improve patient care and the design of processes and systems at Alfred Health. He has completed fellowship training in both intensive care medicine and emergency medicine, as well as post-graduate training in biochemistry, clinical toxicology, clinical epidemiology, and health professional education. He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives.Īfter finishing his medical degree at the University of Auckland, he continued post-graduate training in New Zealand as well as Australia’s Northern Territory, Perth and Melbourne. He is on the Board of Directors for the Intensive Care Foundation and is a First Part Examiner for the College of Intensive Care Medicine. He is also a Clinical Adjunct Associate Professor at Monash University. He is a co-founder of the Australia and New Zealand Clinician Educator Network (ANZCEN) and is the Lead for the ANZCEN Clinician Educator Incubator programme. Anaerobes: Consider brain abscess, elderlyĬhris is an Intensivist and ECMO specialist at the Alfred ICU in Melbourne.H Influenzae: (3%) – Head trauma with CSF leak, otitis, sinusitis, anatomical defects such as dermal sinus tracts.Staphylococcus: Penetrating skull injury, ear or neuro operations.N meningitidis: (30%) – Children and adolescents.Pneumococcus: (40%) – Otitis media, head injury, pneumonia, immunocompromised.Lymphocytosis, variable protein elevation and normal glucose.Aseptic meningitis (Generally accepted as mainly viral meningitis).Sickle cell disease – Capsulated organisms.Humoral or asplenic – Neiserria, enterovirus.N meningitidis, s. pneumonia, listeria, klebsiella, s. aureus.extended culture (Listeria, Cryptococcus).xanthochromic index with spectrophotometry (in SAH).less than half serum in infections (bacterial, Tb and fungal infections) and vasculitis and sarcoidosis.increased in CNS inflammation (including CSF drains and blood in CSF).oligoclonal bands in multiple sclerosis.increased in GBS, vasculitis and sarcoidosis.increased in infection: Tb > bacterial > viral.mixed lymphocytosis/monocytosis in GBS and status epilepticus.lymphocytosis: viral, TB, cryptococcal and listerial infections.polymorphonuclear leukocytosis: bacterial infection.in traumatic tap classically taught to expect 1 WCC : 500 RCC (if normal in peripheral cell counts) but this is not reliable.yellow with xanthochromia (this takes 6-12 hours to develop after blood enters CSF). 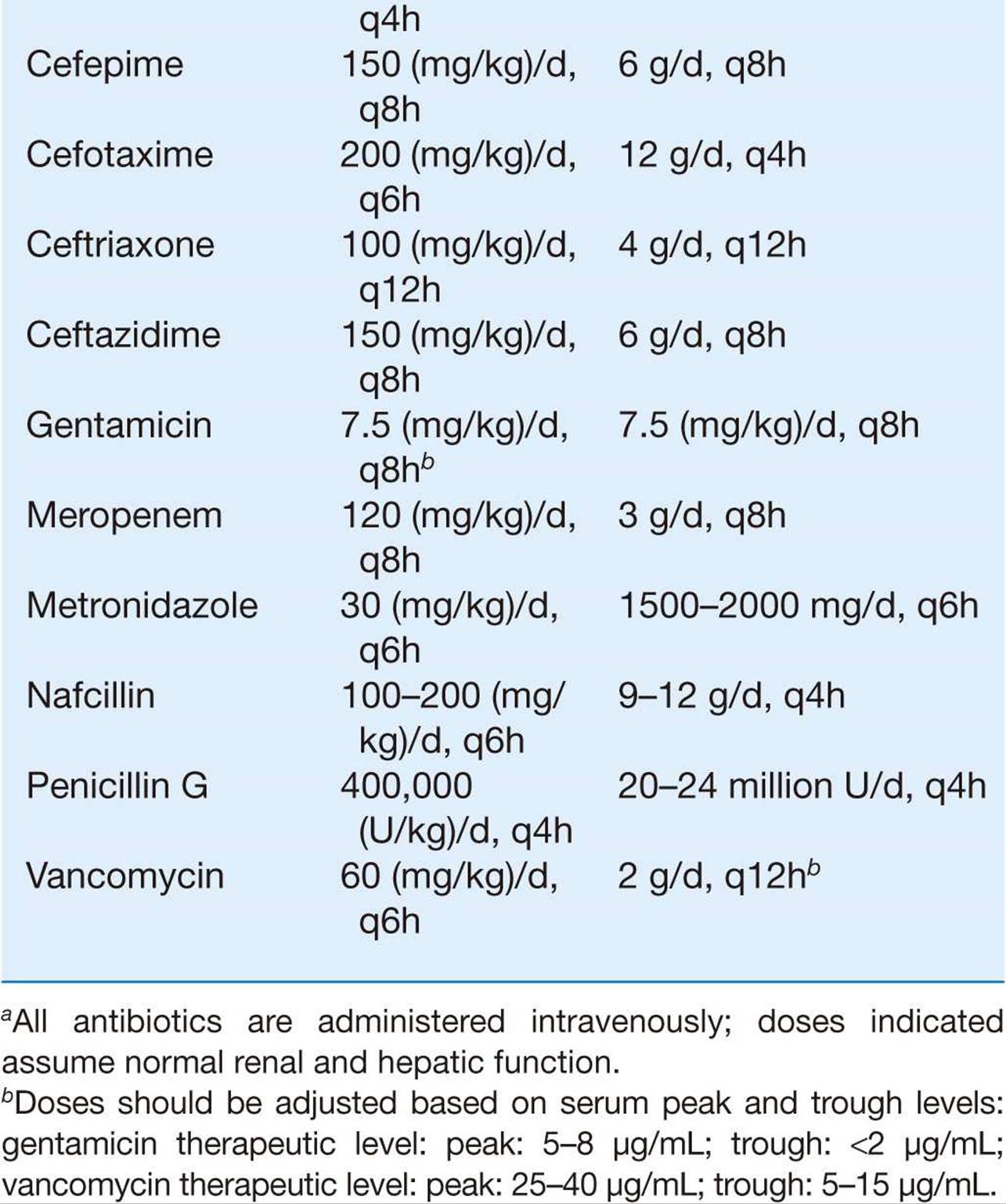 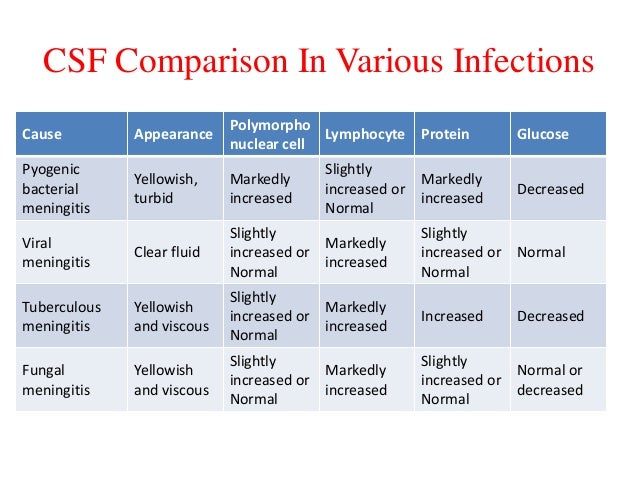
blood stained with SAH and traumatic taps.cryptoccal antigen and Indian ink stain.It may also help exclude the diagnosis of bacterial meningitis especially in cases in which no microorganisms can be cultured.Ĭopyright © 2014 Elsevier Inc. Since the CSF glucose and blood glucose values are promptly and easily obtained from a lumbar puncture, the CSF/blood glucose ratio should be considered as a timely diagnostic indicator of bacterial meningitis. This study suggests that the CSF/blood glucose ratio may be a better single indicator for bacterial meningitis. While neutrophil-predominant pleocytosis and a decreased glucose level in CSF can predict the presence of bacterial meningitis, the CSF/blood glucose ratio is more precise (optimal cut-off=0.36, sensitivity=92.9%, specificity=92.9%, area under the curve=.97) even after administration of antimicrobials prior to examination in the emergency department. We identified 15 patients with bacterial meningitis and 129 patients with aseptic meningitis. The diagnosis of meningitis is made when the white blood cell count in CSF exceeds 5 cells/μL, while the diagnosis of bacterial meningitis additionally requires the growth of a pathogen from a CSF culture or the identification of a pathogen in Gram staining of CSF specimen. This is a single-center, retrospective review of medical records to determine which emergency laboratory CSF test results are useful for predicting bacterial meningitis. Although the lumbar puncture is widely used as a diagnostic tool for bacterial meningitis, it remains unclear which value in cerebrospinal fluid (CSF) analysis in emergency laboratory tests precisely predicts the presence of bacterial meningitis. Bacterial meningitis is an emergent disease requiring prompt diagnosis and treatment with appropriate antimicrobials.
0 Comments
Leave a Reply. |



 RSS Feed
RSS Feed
